Over the past decade, technology has rapidly evolved across the health care landscape. With this comes the advent of digital health – the use of information technology, electronic communication tools, and processes to deliver health care services. Applications of digital health that are commonly used across the industry include: telehealth, clinical decision support, and wearable devices.
Telehealth services have increased since the COVID-19 pandemic. Examples of telehealth services include scheduled visits through secure patient-to-provider video conferencing platforms, remote patient monitoring, health education over phone conversation, and medical information sent through a secure platform.1 The Assistant Secretary for Planning and Evaluation of United States of Health and Human Resources did a trend analysis based upon the Census Bureau’s Household Pulse Survey 2021 to see the use of telehealth services in different populations.2 Based upon the trend, the highest rates of telehealth visits were Medicaid patients (29.3%) and patients earning less than $25,000 annually (26.7%). Benefits, especially to this population, include reduced costs for dependent care, transportation, convenience, and time savings.3 Telehealth is demonstrated to reach a larger population, allowing a greater impact for services rendered.
Clinical decision support has been used by providers and pharmacies to help make decisions about patient’s clinical diagnosis and adverse effects from medications. Figure 1 explains how clinical decision support systems are utilized. Patients and providers will input patient’s demographics, allergies, medication lists, and pertinent information that can be included in the Electronic Health Records (EHRs). From here, the data is input into the clinical decision support that will use algorithms from evidence-based resources to recommend a clinical diagnosis for the patient. The ultimate decision from the clinical decision support would be the provider.
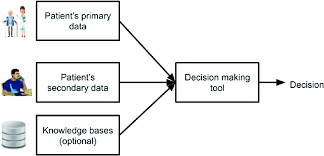
Figure 1: Diagram of Clinical Decision Support Module4
Wearable devices for health services have been trending for the last decade. Smartwatches such as Apple watches, Android watches, and Fitbits have shown common applications for healthy habits and patient monitoring. For those who only see a provider annually, it is an option to self monitor their health. Many watches have applications to track exercise, walking distance, heart rate, irregular heartbeat, blood oxygen levels,ovulation cycles, and sleep patterns. Wearable ECG monitors can track irregular heart rhythms. Wearable blood pressure monitors are available to check for blood pressure. Wearable blood glucose monitors have made it easier for patients to check on blood sugar. These device allow the blood sugar report to be sent wirelessly to a device or to a smartphone that allows providers to access blood sugar trends.
Figure 2: Smartwatches Benefits5
Digital Health is expanding exponentially. The resources that are available can be utilized to reach a broader number of patients. Sites can:
- Utilize telehealth services, such as secure video chat with patients to ensure that appointments are not missed and have easy access.
- Send refill reminders can be sent as a text message to the patients for adherence.
- Send a weekly education advising tips for specific disease states to encourage patients for positive health outcomes.
- Provide affordable wearables to monitor their heart rate, walking steps, and calories to promote healthy habits.
The data that is provided from these resources, such as metrics on refills/adherence, health impacts, etc., can be shared with Dispensary of Hope to see the impact that digital health has on a larger population of patients.
Digital divide is the idea of the gap of having access to technology and using the information to utilize the technology.6 With the exponential increase and demand in use of digital health, we need to keep in mind the patient population. Sites that are in network with Dispensary of Hope reach out to patient populations that are uninsured and the Federal Poverty Level of less than 300%. Social determinants of health, such as income, health literacy, generational gap, and education, can provide a gap to the patient population when trying to provide these resources.7 As resources are being readily available, adding telehealth services to a practice can help connect patients to providers, reducing some social determinants of health barriers for this population.
Azmaan Lakhani, 2022 PharmD
Belmont University College of Pharmacy
Adapted from a Dispensary of Hope Newsletter
Resources:
- Tuckson RV, Smith MR, Watterberg KL, et al. Telehealth. N Engl J Med. 2017; 316(16):1585-1592. Doi: doi/10.1056/NEJMsr1503323
- Karimi M, Lee EC, Couture SJ. National Survey Trends in Telehealth Use in 2021: Disparities in Utilization and Audio vs. Video Services. Updated February 1, 2022. Accessed March 28, 2022. https://aspe.hhs.gov/sites/default/files/documents/4e1853c0b4885112b2994680a58af9ed/telehealth-hps-ib.pdf
- Snowden A. Digital Health: A framework for healthcare transformation white paper. HIMSS. Updated April 13, 2020. Accessed March 22, 2022. https://www.himss.org/resources/digital-health-framework-healthcare-transformation-white-paper
- Peiffer-Smadja N, Rawson TM, Ahmad R, et al. Machine learning for clinical decision support in infectious diseases: a narrative review of current applications. Clin Microbiol Infect. 2020;26(8):1118. doi:10.1016/j.cmi.2019.09.009
- Sinhasane S. Wearable technology: The Coming Revolution in digital health. Mobisoft Infotech. Updated May 28, 2018. Accessed March 22, 2022. https://mobisoftinfotech.com/resources/blog/wearable-technology-in-healthcare/
- Valu M. Understanding the digital divide and ensuring access for all. Updated March 30, 2021. Accessed March 28, 2022. https://www.himss.org/resources/understanding-digital-divide-and-ensuring-access-all
- Social determinants of health: healthy people 2030. Accessed March 28, 2022. https://health.gov/healthypeople/objectives-and-data/social-determinants-health

